Every month, I’ll go into detail about a specific procedure that I perform. This month I’ll be discussing balloon sinuplasty.
Balloon sinuplasty is a fairly new procedure that has only been in existence since 2005. The purpose of the procedure is to widen the openings into the sinuses so that they are better able to drain. In essence, it’s a plumbing procedure: narrow drainage pipes are widened.
The procedure was inspired by cardiac angioplasty, a procedure in which a balloon is used to open blocked arteries around the heart. In balloon sinuplasty, the same idea is used to open blocked or narrow openings into the sinuses to help treat and prevent sinus infections.
There are two main groups of patients who can benefit from balloon sinuplasty:
-
Patients with chronic sinusitis (sinus infection lasting more than 3 months and not improving with antibiotics)
-
Patients with recurrent acute sinusitis (more than 3-4 sinus infections each year which clear up in between)
Most adult and teen patients can have the procedure done in the office with or without mild sedation. Younger children need to go under anesthesia.
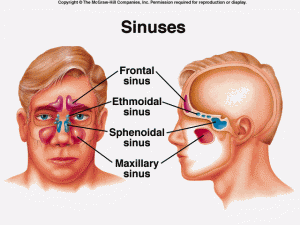
A total of 6 sinuses can potentially be opened using the balloon: 2 maxillary sinuses, 2 frontal sinuses, and 2 sphenoid sinuses. Review the anatomy of the sinuses HERE.
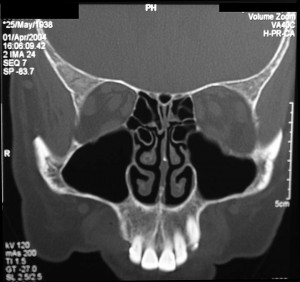
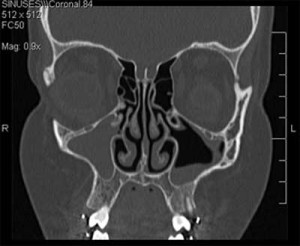
For chronic sinusitis patients, the specific sinuses I open depend on what your CT scan looks like. For recurrent acute sinusitis patients, the CT scan is often normal if it is done between infections.
In recurrent acute sinusitis patients, I dilate sinuses depending partly on the patient’s story (i.e. is pressure on both sides or on one only?) and partly on the appearance of the sinus openings during nasal endoscopy. Frequently, there is a lot of swelling around all the sinus drainage pathways in these patients, and I will go ahead and dilate all 6 sinuses. My opinion is that if you are going to come in and get sedated and have your nose numbed, it is better to err on the side of opening all the sinuses than risk needing to come back in the future to finish the job. I discuss this in advance with patients and I’ve found that all have agreed with me.
How does the procedure work in the office? First, one hour before you come in, you’ll take an oral pain medication (usually Norco). Once you arrive, I’ll get your consent for the procedure and then administer a shot of sedating medication. Then, I’ll spend about 30 minutes getting the inside of your nose very numb while the sedation is taking effect.
There are 3 steps to the numbing process: first spraying numbing medicine and decongestant in your nose, then squirting a gel with numbing medication around the sinus openings, and finally injecting more numbing medication around the sinus openings (patients generally do not feel the injections at all because of what has already been done). I have found that patients tolerate the procedure very well with this protocol.
After all this, I can begin the procedure. The balloon device has a thin guidewire with a light on the end of it. Once I insert the wire correctly into the sinus, I can see the glow of the light through the skin. Then, I advance the balloon over the guidewire until it is sitting across the opening into the sinus. The balloon is then inflated with highly pressurized water by my nurse to widen the sinus opening. During the inflation, patients will feel pressure and discomfort for several seconds and hear “snap, crackle, and pop” noises as the bone around the sinus is widened and remodeled.
Here is an animation of the balloon dilation of a left maxillary sinus:
http://www.youtube.com/watch?v=oCZJ3wfaTLI
I’ll then move on the remaining sinuses that are appropriate for the procedure and repeat the process. The entire balloon procedure can be as quick as 5-10 minutes but can last longer if one or more of the sinus openings are narrow and difficult to cannulate with the guidewire.
After the procedure, I’ll place some gauze soaked in Afrin inside the nose for a few minutes to help stop any bleeding, and then patients can go home with someone to drive them.
Patients are usually mildly sore for a few days after the procedure and there is sometimes some mild bleeding the rest of the day. Patients will feel stuffy and congested for about 1 week after the procedure and then will start to open up in the following weeks.
I’ve continually been surprised by how well patients do after this procedure. I tend to be skeptical about new procedures and devices because honestly most of them are overly hyped by sales reps. My skepticism has been proven wrong by the 30 or so balloon procedures I’ve done in the past year. My patients have almost all been very happy and feel better afterwards, and they generally find the procedure very tolerable in the office, especially with the sedation protocol I’ve developed.